This is part of a series of blog posts examining how Patient Support Services teams can deliver an outstanding patient experience.
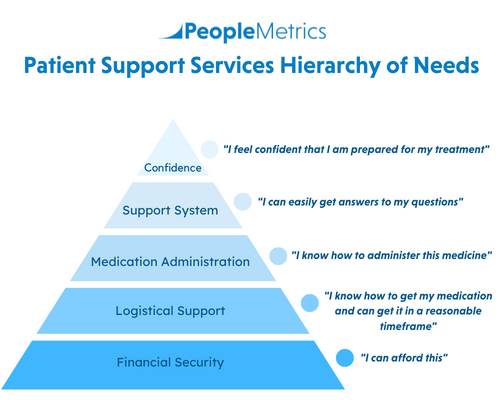
To help Patient Support Services teams measure and improve the patient experience, PeopleMetrics has developed a model called the Patient Hierarchy of Needs.
This model includes five core patient needs and 15 questions that link to each need:
This model is based on Maslow’s Hierarchy of Needs, whereby certain needs must be fulfilled before higher order needs become relevant.
In previous blog posts, we've covered 3 fundamental patient needs that need to be fulfilled before they onboard onto a new medication:
Once these key patient needs are fulfilled, patient support services teams can truly add unique value to the patient experience by providing a support system - can the patient easily get answers to their questions before they onboard onto their newly prescribed medication?
Level 4: Support System
The crucial fourth level of patient needs - support system - is shown in the pyramid below:
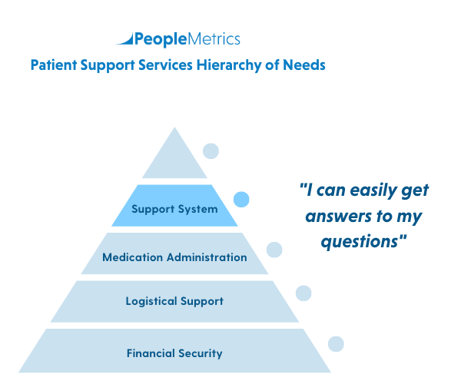
Patients have a variety of questions beyond the basic ones we have covered in previous blog posts. This can include questions about their finances, their treatment, and their condition.
Patient support services teams have the opportunity to provide vital direction here.
Whether you can answer a patient's question or not, the key is to stay consistent
Providing support to patients can be tricky because there are numerous legal boundaries to what patient support services teams are permitted to discuss with patients. Patients aren't usually aware of these limitations, however, so your approach to answering these types of questions can have a significant impact on the patient experience.
This is true if you have an in-house team or if you use a partner Hub; and is especially important if the medication is for a rare disease. It's a huge responsibility and opportunity to add incredible value.
For the questions your team can answer, you need to make sure that everyone on your team is providing consistent answers to each patient.
For the questions you cannot answer, make sure that your team has a consistent process for directing patients to doctors, advocacy groups, or other resources that are able to further assist them.
Not only can it mean the difference between onboarding or not... it can and does change lives.
Ask these survey questions to measure your support system's effectiveness:
Unlike the past few patient needs where only one or two questions were required to measure effectiveness, providing a support system is more involved and requires more answers from patients about their experience.
Let's start with two questions that apply to any type of drug - from rare disease to mass market medications.
The first uses the same 5-point agreement scale that we've referenced in previous blog posts (5 = "strongly agree," 1 = "strongly disagree"):
- I have a clear understanding of the patient support services available
This is a broader question that provides an overall indication as to how much patients understand what is available to them.
The next question is around communication, which is fundamental for providing a patient support system:
- How would you describe the level of communication that you received from [COMPANY] during your onboarding (including emails, mailings, and communications from your Case Manager?)
- Not enough communication
- Just the right amount
- Too much communication
You'll notice that we mention case managers in this question. If you have case managers, use this question as-is. If you don't have case managers, this question is still relevant. Getting your communication cadence correct builds the foundation of the support system you're providing for your patients.
Measuring case manager performance
If you have case managers, you should ask the following questions about patients' interactions with these key members of your team.
The first case manager question is overall satisfaction. It is asked on a 5 point scale (1 = "not at all satisfied," 5 = "extremely satisfied"):
- Please rate your satisfaction with your case manager, [CASE MANAGER NAME]
Next, there are two questions that dig into case manager performance:
- Based on your interaction with [CASE MANAGER NAME], how strongly would you agree that your case manager provided you with accurate up-to-date information?
- Based on your interaction with [CASE MANAGER NAME], how strongly would you agree that your case manager is accessible when you have questions or concerns?
Accuracy and timeliness of information provided by case managers is key to any effective support system.
Patients also need to feel like they can count on being able to contact their case manager when they need to. A support system that isn't accessible won't be very effective.
Measure case manager performance consistently, and make sure you follow up with any patient who feels their case manager is difficult to reach.
Questions to inform a differentiated patient experience
The last two questions focus on what your best case managers are doing to exceed patient expectations and provide a differentiated experience:
- Thinking of your interactions with [CASE MANAGER NAME], was there an instance where they exceeded your expectations?
- Yes
- No
If the patient answers "Yes," they are asked this follow-up question:
- Please tell us specifically what they did
This is an open-ended question that provides patients the opportunity to share in their own words what makes their case manager interactions special.
This is gold.
This is where you can truly understand what makes a great case manager. It's where you can identify what ALL case managers should be doing to make the patient experience the best it can be. It's where you get your training material for new case managers. It gives you a clue on what to look for when hiring new case managers.
Use this information to make your case managers the best they can be, and set yourself apart from the competition with a differentiated patient experience.
Providing an effective support system for patients is not easy and involves many components - but it's worth it, and here's why:
After a patient feels they have a support system where they can get answers to their questions, they move to the top of the pyramid - the ultimate patient need - confidence.
The final blog post in this series will dive into confidence and its massive impact on patient onboarding and adherence.
○ ○ ○
Read all of the blog posts in this series:
- Introduction to PeopleMetrics' Patient Hierarchy of Needs
- Level 1: Financial Security
- Level 2: Logistical Support
- Level 3: Medication Administration
- Level 4: Support System
- Level 5: Confidence
○ ○ ○
About the Author
Sean McDade, PhD is the author of Listen or Die: 40 Lessons That Turn Customer Feedback Into Gold. He founded PeopleMetrics in 2001 and is the architect of the company’s customer experience management (CEM) software platform. As CEO, he guides the company’s vision and strategy. Sean has over 20 years of experience helping companies measure and improve the customer experience. Earlier in his career, he spent five years at the Gallup Organization, where he was the practice leader of their consulting division. His company offers CEM software with advanced machine learning solutions and hands-on analytical support to help companies make sense of their CX data. Sean holds a Ph.D. in Business Administration with a specialization in marketing science from Temple University in Philadelphia. He has published eight articles in peer-reviewed scholarly journals and has taught over 25 marketing classes. Sean was named a 40 under 40 award recipient of the Philadelphia region. He is an active Angel Investor, including investments in Tender Greens, CloudMine and Sidecar.
Topic: Pharma CX